William Reyes was born on Sunday December 9th, 2018 at 1:32 pm. He came out with gusto, and has quite the impressive birth story!

As many of you know, I have had an official diagnosis of cholestasis since 30 weeks due to elevated bile acid levels.
I also had cholestasis with my first pregnancy. This diagnosis has a high risk of stillbirth.
Since my bile acid levels spiked super high this pregnancy, we had a plan to induce this pregnancy at 36 weeks.
Well, 34 weeks rolled around and something felt off. I couldn’t shake the feeling.
William just wasn’t moving around in the same ways that he had been.
He was passing his biophysical profile tests. All looked good on paper, but to Mama it was different. I just had a weird feeling.
I wrote about it in this post, but in a nutshell, my perinatologist trusted in me. My OB trusted me. My husband trusted me.
They scheduled an induction with the hospital at 34 weeks, and told them to move forward with it if I were to show up and make the call that it was time.
Saturday morning I knew it was time. I was 34 weeks 1 day and we headed to the hospital to trust my Mama gut.
I am so glad we did…
The plan was to get there Saturday and get my first of 2 betamethasone (steroid) shots for William’s lung development. On Sunday, I’d get the second shot, and then be induced (around 1 pm).
William had other plans, however.
When we got to the hospital, I was 2 cm dilated (as I had been the week before).
Things quickly changed, however, with no assistance.
Later that evening, I was having a lot of contractions that were getting stronger.
By 4 am in the morning, the contractions were strong enough to ask for a check. The doctor came in and checked me. I was 4 cm dilated now, 80% effaced, and William was not engaged yet (-4 position).
What amazing news. William was making it clear that he was coming out. No induction needed!
I was transferred to labor and delivery later that morning. They checked me again and I was 6cm, 100% effaced, and William was -2 position.
My second betamethasone shot was ordered up early.
We got the second shot in, and then waited to see how quickly my body was going to progress.
At my next check, we went ahead and broke my water. There was meconium. Not the best news, as that’s dangerous for baby to inhale, and one of the reasons cholestasis babies are induced before 37 weeks.
I was informed that NICU would be taking him immediately, suctioning his nose and mouth, and that I might not hold him first thing.
30 minutes later, I was also given the lowest dose of pitocin just to help speed things up, since we knew we wanted William to make his appearance that day.
I think that was all around 11/11:30am. William was born at 1:32pm.
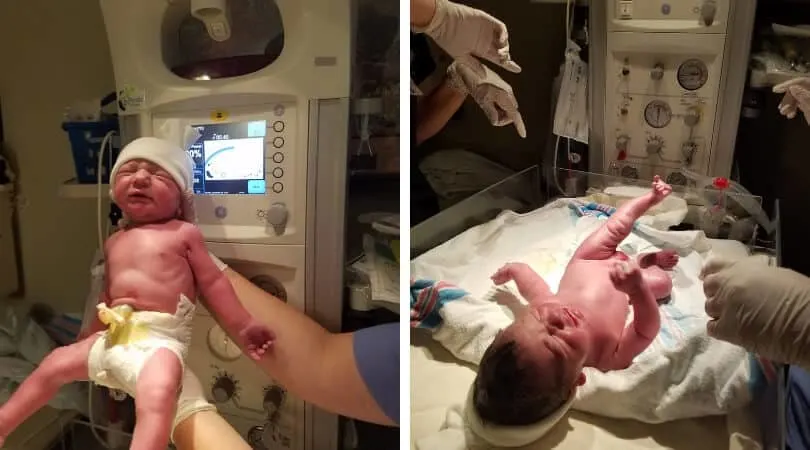
It was all very fast!
I’d been thinking about if I wanted an epidural or not. I’d had some bad dreams about the epidural.
There are small risks associated with being on blood thinners for antiphospholipid syndrome and getting an epidural.
I also knew that they were waiting long enough for the blood thinners to be out of my system before giving me an epidural. There was nothing to worry about.
But, in my research, I was intrigued by no epidural.
I was drawn to the idea of a faster delivery, the appeal of knowing when to push instead of just pushing when told to. The appeal of letting gravity do its job, instead of being stuck lying in bed. The appeal of a faster recovery.
So, I turned down the epidural and put my brave shoes on. I was nervous though. I figured I was a bit crazy, but I had my mind made up and was going for it.
I used a birthing ball for most of my labor. I held my husband’s hand. We played music and a word game that we like to do together on the iPad. I had decent breaks in between contractions.
So, while the contractions were yell worthy, I figured we weren’t close to pushing yet since I had time in between. My nurse didn’t seem concerned yet.
But then it happened. Transition time. Baby was coming out. I HAD to push. My body wasn’t giving me a choice.
Yet, I was told not to push. My doctor wasn’t there yet. The NICU team wasn’t there yet. I couldn’t push. And yet I couldn’t not push. The pain was unreal in that moment as I tried to fight my body’s natural urge.
My husband took such good care of me through the contractions and birth. I don’t think I could have done it without him. He kept me focused and was so amazing.
Finally, I was told to push. I needed some refocusing as I was in so much pain trying to hold him in. And then in 2 big pushes, and 2 little ones (as my OB put it), I got William out.
He immediately cried. I was so glad to hear that cry, but also so scared due to the meconium. I knew he needed NICU attention. I also got to hold him briefly as they cut the cord.
Then NICU did their thing. My husband went and watched.
I on the other hand had more to do. I delivered the placenta, and then had to have a shot to numb me, and stitches for a first degree tear. Not pleasant, but I made it through.
William was then doing so good, the NICU team let me hold him for a few minutes before taking him away.
We visited him as soon as they’d let us.
In the NICU we were told that he was doing great breathing, and regulating his temperature. His blood sugar was a bit low so he’d be on IV fluids.
He was on a feeding tube for about 24 hours if I remember right. Once he started eating, they’d wean him off of the fluids and remove the feeding tube.
The NICU is daunting. These babies are so tiny (although at 6 lbs 3 oz William is a big preemie)!
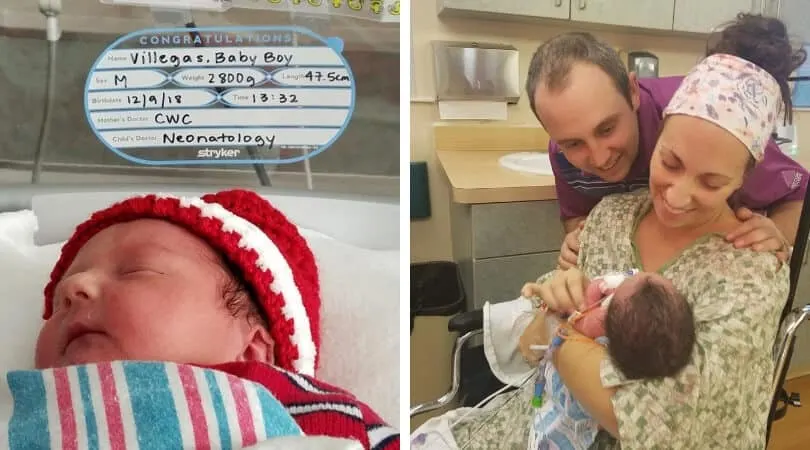
The babies are hooked up to monitors and IV’s. The wires are overwhelming when you are trying to just hold and snuggle on your little one.
Children under 6 aren’t allowed in. That means that, until William comes home, Caroline can’t even meet him.
It’s hard. So insanely hard.
Today is Thursday. He’s still in the NICU and likely has several more days.
They are cautious and slow for good reason.
He’s doing great, though!
Today (12/13) he was weaned off of IV fluids and is taking 50mL for each 3 hour feeding.
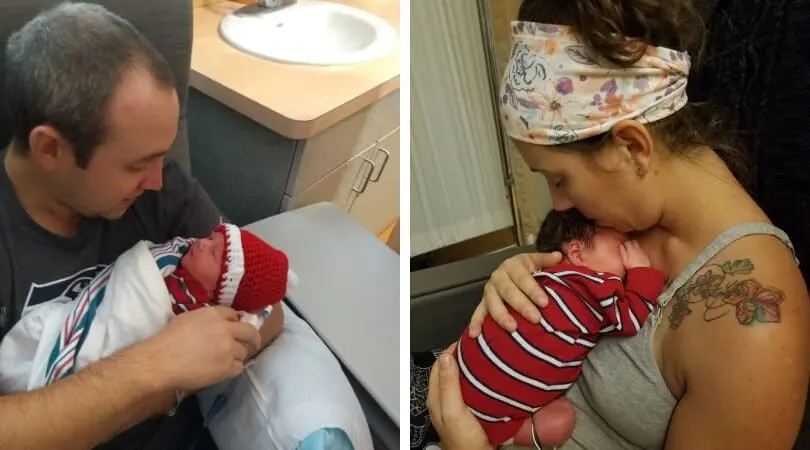
He’s had a couple of breathing “events” they call them. It happens when eating. His body can’t coordinate eating and breathing at the same time, basically.
I’ve never seen one happen, and they are few and far between. It sounds like when an “event” happens, however, they keep the baby for 3 more days.
So, we are at least 3 days out from taking him home.
We visit as often as we can.
I was discharged Tuesday morning and it’s back to normal life. My husband is home for 2 weeks as we try to manage taking care of Caroline, her activities (school, swim and gymnastics), grocery shopping, and cooking. The normal things all have to happen.
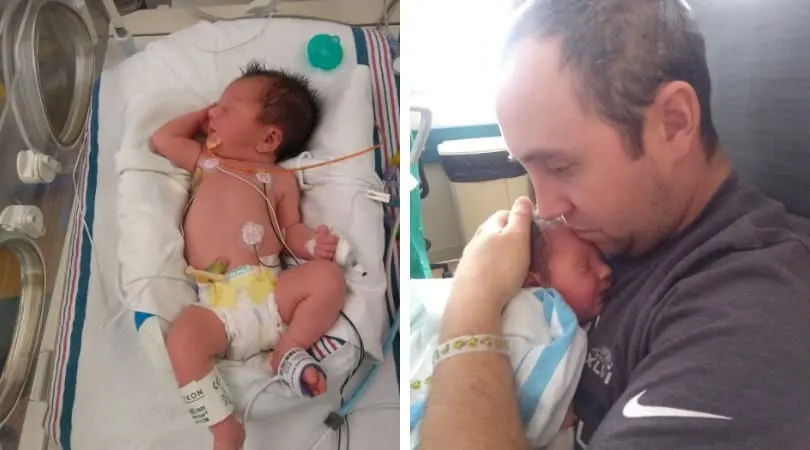
And then I have to now pump every 3 hours at least to keep my supply up. In addition to that, we also try to visit William whenever we can.
There’s just not enough time to do it all. By the time I get home from visiting him, then pump, and take care of one little thing, it’s time to go back.
I wish I could be with him more, but I’m having to realize that I can’t do as much as I want.
Soon, he’ll be home and in our arms. Taking care of a feeding won’t require driving to him and signing into the NICU. Caroline will get to meet her baby brother. Soon!

In the meantime, this Mama is forever grateful that I listened to that voice telling me to go in. We won’t ever know what would have happened had I not.
Thank goodness I had such a great support system (doctors and husband) that trusted me.
William Reyes Villegas, welcome to the world sweet boy.

